Preventing falls is about balance – physical, medical, and nutritional
Anyone can fall. But according to Health Canada, seniors fall more often, and the consequences are more serious. More than one in three Canadians over 65 will fall each year. Half will have an injury that reduces their mobility and independence.
Physical changes that occur with aging increase the risk of falling. Muscles lose strength and flexibility. Balance reflexes slow down. Vision is poorer. Health conditions like arthritis, stroke, and Parkinson’s disease increase the risk of falling. What’s more, some prescription medications, such as drugs to control blood pressure, interfere with balance.
These risk factors are cumulative — the more risk factors you have, the greater the risk of falling. Recognizing these factors is the first step in preventing falls. The next step is adjusting home and lifestyle to reduce as many risk factors as possible, and stay safe.
Keeping a healthy balance of physical, medical, and nutritional factors in your life will help you to live an active life and prevent falls.
Exercise
Exercise is one of the keys to preventing falls. It maintains your strength, endurance, and bone health. It also contributes to balance. There are many ways to exercise – from dancing or walking to armchair fitness. You can go to a gym, but you can also get your exercise at a shopping mall, a senior centre or just at home. Talk to your health care provider about the best program of exercise for you.
Many seniors enjoy walking their pet as a form of exercise. One caution: be careful around dog leashes, which can cause falls.
Safety aids and supports
Have your vision and hearing checked regularly. Wear your glasses or hearing aid(s). Wear good supportive footwear with closed heels and toes, and of proper size.
Use an aid for walking if you need it. The new Nordic-style walking poles are becoming very popular.
Keep your home well-lit. Make sure stairways have good lighting. Install a night light at the top of the stairs. Keep a flashlight near the bed in case the power goes out.
Don’t stand on furniture to reach a shelf. Instead, use a sturdy stepladder. If you have been having balance problems, ask for help. Put items that you use a lot on the lower shelves. It is easy to ‘overbalance’ and fall if you are lifting something heavy over your head.
Install handrails and grab-bars in bathrooms and stairways. When you carry things up and down the stairs, always keep one hand free so that you can hold on to the handrail.
View all of your safety aids and supports as sources of strength to help you do things independently, not signs of weakness.

Maintaining your balance
Talk to a doctor or pharmacist about the possible side effects of any medicine you take, especially drowsiness or dizziness. Be sure to ask about its effect when combined with other medicine, food or health supplements you take. If you take medicine for blood pressure, ask your doctor or nurse to measure your blood pressure both while sitting and standing. Some people find that their blood pressure may drop when they stand, which can make them dizzy. An adjustment to the dosage of medication may be required.
You can help to prevent morning dizziness by sitting on the edge of the bed for 10 seconds before you get up.
Take good care of your feet. Make sure that any corns, calluses, or long nails are trimmed. Get your feet checked regularly, especially if you have diabetes.
Healthy diet
A healthy diet maintains strength, balance, and resistance to disease. Some people find it helps to eat smaller meals throughout the day rather than the traditional ‘three squares’. If you drink alcohol, watch out for its effect on your balance and walking. This goes double if you are also taking medications.
Tips for controlling hazards at home
- In winter, keep steps and walkways clear. Use salt or sand on ice.
- When walking outdoors in winter, put tips on canes and other walking aids that help prevent slipping.
- Wipe up any spills as soon as they happen, especially on ceramic floors.
- Don’t leave clutter on the stairs.
- Remember to slow down, even if you are late. In a rush, it is easy to overlook hazards.
About the Author
Compiled by the Seniors’ Health Division, Canadian Physiotherapy Association
Click Here for print PDF file – Safety – Preventing falls is about balance
Do you know how to compensate when you move?
by John C. Griffin, MSc
As people get older, they lose mobility. It is the first area where most older adults become impaired or disabled. In fact, De Brito and colleagues (2013) found that the ability to rise from the floor was a significant predictor of mortality in 51- to 80-year-olds. That means that people who could not get up after sitting on the floor were more likely to die early than others in their age group.
You have a role to play in preventing mobility loss
When you start to have trouble with certain tasks or activities, it is called a preclinical stage. The preclinical stage is a critical time for intervention. You can slow this down! Mobility problems can take one of three courses:
- Cessation: The worst option is to stop doing things that you used to do. For instance, someone who is starting to have trouble reaching up over their head might give up a favourite sport, like tennis or squash. This could lead to a more sedentary lifestyle, and that would lead to losing even more mobility.
- Retraining or repairing: It is often possible to regain performance in the area where mobility is becoming difficult. So many older adults are reluctant to visit a physiotherapist when they have a joint or muscle problem. But these health professionals can help you to regain mobility and step back into your active lifestyle. Or, they might help you to modify a task or activity so that you can still do it safely. This is called compensation.
- Compensation: Compensation can be both good and bad. If you alter a movement pattern so that you can still do it, but in the wrong way, it could lead to injury. For instance, someone who had weak leg muscles might start to bend from the waist to lift things, instead of bending their knees. That’s a sure-fire way to injure your back. On the other hand, a well-designed modification to a task or activity can slow down mobility decline. A good example of safe compensation is using Nordic poles when hiking to help with balance and reduce knee strain.
A good compensation strategy for getting up off the floor
Aging makes it harder to get down on the floor to do things like play with a child, clean out a cupboard, or do a floor exercise. We may have decreased upper and lower body strength, less range of motion, balance issues, or all three. We fear that we cannot get back up again without looking clumsy or losing our balance.
But researchers have described a technique that makes getting up off the floor much easier (Moxley, 2012). It might work for you, unless you have had a total knee or hip replacement or some other serious issue.
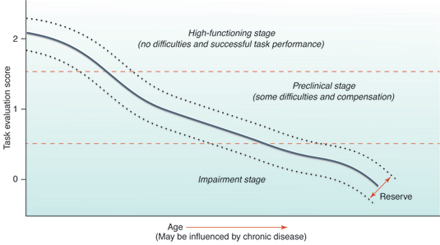
This chart shows the decline of physical function with age
How to do it:
- From your side, roll onto your stomach.
- Bring your knees in one by one to a position of all fours.
- Bring one leg up and forward under your chest, with your foot on the floor.
- Bring your hand to your thigh.
- Press your hand on one thigh as you bring the other leg up.
For safety: Place a sturdy chair nearby for support or in case you get dizzy.
1.)  2.)
2.) 
3.)  4. & 5.)
4. & 5.) 
References:
de Brito, L.B.B. et al. 2013. Ability to sit and rise from the floor as a predictor of all-cause mortality. European Journal of Preventive Cardiology 2014 July; 21(7):892-8.
Griffin, J.C. 2015. Client-Centered Exercise Prescription. Third edition. Champaign, Il.: Human Kinetics, www.HumanKinetics.com.
Moxley, C. 2012. Floor freedom: How to get up from the floor. Functional U (ICAA) 10(5): 1-10.
About the Author
John C. Griffin, MSc, , is an award-winning retired professor, private consultant, speaker, writer, and coach. He has authored more than 100 publications, including Client-Centered Exercise Prescription and chapters in the grade 12 Exercise Sciences and Healthy Active Living textbooks. Recently, he has conducted research on the functional mobility of older adults and developed a screening tool and exercise prescription algorithm. John worked with the Canadian Society for Exercise Physiology on the national certification for personal fitness trainers and is a national course conductor and examiner. Working with the National Fitness Leadership Advisory Council, John co-authored the first national standards for exercise leaders in Canada.
Click Here for print PDF file – Active Living – how to compensate when you move

- Categories
Recent Posts

